Argomenti trattati
On Thursday, March 12, 2026, a collaborative effort between Marshall University, Marshall Health Network and Intermed Labs moved into the prototype phase with a project known as the DBS Lead Lock. The initiative grew from surgical practice: Dr. Heather Pinckard-Dover, a neurosurgeon and associate professor at the Joan C. Edwards School of Medicine, identified limitations in existing fixation methods while performing deep brain stimulation procedures. The team framed the work as clinician-driven innovation—a development path that starts with a real-world clinical challenge and builds technical solutions around it. This announcement highlights the combined roles of clinical insight, university-based manufacturing resources, and med-tech commercialization partners in translating operating room needs into tangible devices.
The project’s goal is straightforward yet technically demanding: increase the stability and ease of securing DBS leads during implantation without adding complexity to the surgical workflow. Deep brain stimulation itself is an advanced neurosurgical therapy that treats disorders such as Parkinson’s disease and essential tremor by placing fine electrical leads into precise brain targets, often requiring millimeter-level accuracy. Even minimal micro-movements during lead placement can affect therapeutic outcomes. By focusing on lead fixation, the DBS Lead Lock aims to reduce intraoperative displacement risks and support reproducible positioning while preserving surgeon ergonomics and patient safety.
Why lead fixation matters
Implanting stimulation leads is a delicate choreography of imaging, navigation and manual control. Current stabilization tools help, but clinicians have noted gaps in how leads are handled during critical moments of insertion and anchoring. The team believes that improved fixation mechanics can limit unintended shifts, shorten procedure steps, and potentially lower complication rates. In this context the DBS Lead Lock is being designed as a practical adjunct to existing systems rather than a replacement, integrating with standard surgical workflows and aiming to be manufacturable at scale. The concept emphasizes reliability and repeatability—key attributes for a device that will be used in high-stakes neurosurgical environments.
How the collaboration works
The development strategy pairs frontline clinical experience with prototyping and commercialization capabilities. Intermed Labs brings med-tech product development expertise, while the Marshall Advanced Manufacturing Center (MAMC) supplies fabrication and iterative testing capacity. According to the collaborators, this model preserves the clinical intent of the idea while applying engineering rigor to shape form, function and manufacturability. Ashok Aggarwal, co-founder of Intermed Labs, described the approach as a textbook example of clinician-led problem identification feeding a structured development pathway: concept, prototype, evaluation and eventual regulatory planning.
Prototyping and technical focus
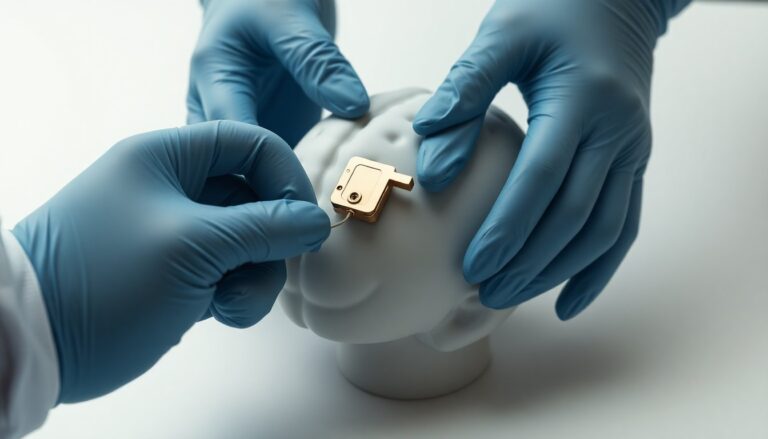
Prototype work at MAMC concentrates on materials, fixation geometry and ease of use under sterile OR conditions. Engineers are testing multiple iterations to balance secure anchoring with gentle handling of leads and minimal footprint on the skull. The team is applying rapid iteration cycles, leveraging advanced manufacturing techniques to refine tolerances and test durability. While specific mechanical details remain proprietary at this early stage, the publicly stated priorities are clear: improve positional stability, simplify the fixation sequence and ensure compatibility with existing implantation hardware.
Commercial and clinical pathway
Beyond engineering, the partnership is preparing for the downstream steps that follow a successful prototype: preclinical validation, human study design, regulatory clearance and commercialization planning. Marshall University leadership emphasized that combining academic medicine with manufacturing and venture-minded partners helps accelerate translation from idea to clinic. Brad D. Smith, president of Marshall University, highlighted the regional and broader impact potential, noting that solutions born from local clinical practice can serve national and international patient populations when developed with robust testing and commercialization strategies.
Next steps and implications
The DBS Lead Lock remains in early-stage development, and collaborators say updates will be shared as prototypes are refined and testing milestones are reached. If the device achieves its objectives, it could contribute to shorter operative times, improved safety margins and more consistent therapeutic outcomes for patients receiving deep brain stimulation. The project also models how surgical observations can be converted into product concepts through university-industry partnerships, with potential applications beyond DBS in other procedures that require precise implant stabilization.
Interested readers and potential partners can follow progress through Marshall University’s medical research channels and Intermed Labs communications. The announcement reinforces a broader movement in healthcare innovation: empowering clinicians to lead problem discovery while enlisting engineering and manufacturing expertise to develop practical, scalable solutions.